The Disparity in GP Workloads Across England
A recent investigation has revealed a stark contrast in the number of patients seen by general practitioners (GPs) across different surgeries in England. Some GPs are seeing fewer than 10 patients per day, while others are handling over 100 appointments daily. This discrepancy has sparked concerns about the quality of care and the potential risks associated with rushed consultations.
Campaigners have raised alarms about the “postcode lottery” that patients face when seeking medical attention. They argue that the pressure on GPs to see more patients can lead to missed symptoms of serious illnesses. Despite the average salary of £140,000 for GPs before tax, many are underutilized in certain areas of the country, highlighting an imbalance in resource allocation.
The findings come as family doctors hint at the possibility of strikes over proposed changes to make it easier for patients to book appointments. These changes include requiring GP surgeries to keep online forms open during their working hours for non-urgent requests. While officials claim this move will be subject to necessary safeguards, the British Medical Association (BMA) warns that the additional workload could be dangerous if not properly managed.
Health Secretary Wes Streeting has pledged to stand firm on the changes, despite the BMA’s threat of a formal dispute. The BMA argues that the current system does not provide adequate safeguards or additional staff to handle the expected increase in online requests. Meanwhile, NHS bosses describe the BMA’s safe limit of 25 appointments per day as “arbitrary.”
Case Studies of GP Practices
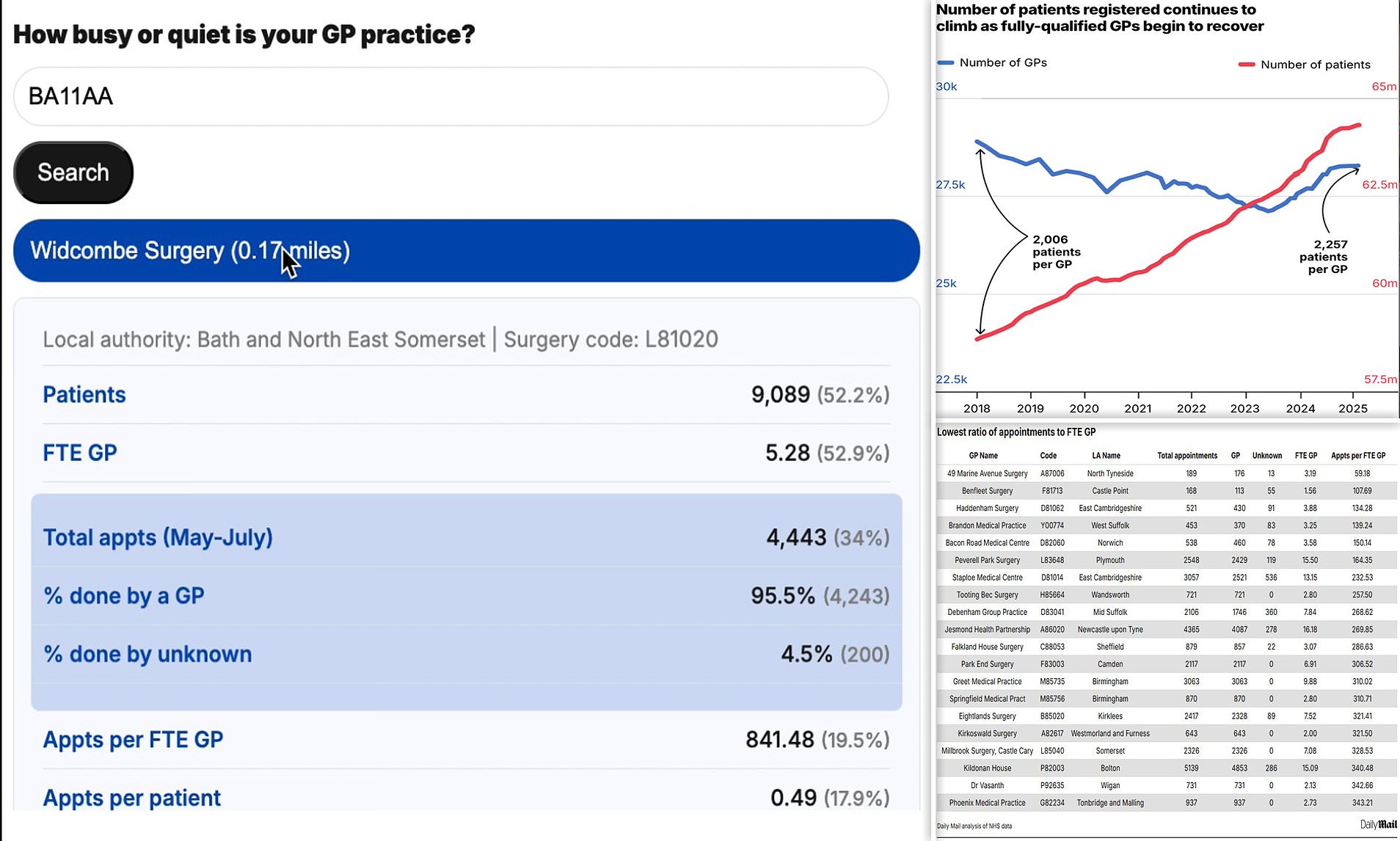
One of the quietest practices identified was 49 Marine Avenue Surgery in Whitley Bay, which recorded only 189 appointments over a three-month period. However, this figure may be skewed due to a merger and limited operational days. Another example is Benfleet Surgery in Essex, which saw just 168 appointments despite having 2,547 patients on its books.
On the other end of the spectrum, the Old School Surgery in Canterbury recorded an impressive 9,536 appointments over the same period. With only one FTE GP, this would equate to approximately 149 appointments per day. Such high workloads raise concerns about the sustainability of the current system and the well-being of GPs.
NHS Digital emphasizes that the figures they publish do not fully reflect the total workload of GPs. In addition to patient consultations, GPs also manage triage requests, process prescriptions, and carry out administrative tasks. They may also visit care homes and attend training sessions.
Concerns About Access and Efficiency
Dennis Reed from Silver Voices highlighted the disparities in access to GP services across the country. He noted that some practices are overwhelmed with patients, while others appear to have very few appointments. This inconsistency has been exacerbated by recent changes to GP availability, leading to calls for improved access and better management of resources.
Shimeon Lee from the Taxpayers Alliance pointed out that the current funding model for GPs, based on a per-patient basis rather than per-appointment, may not be delivering value for money. He suggested that ministers should consider matching busy and quiet practices to ensure a more efficient distribution of patients.
Despite efforts to recruit more GPs, the number of full-time GPs in England has declined over the past decade. Many are retiring early, moving abroad, or leaving for the private sector due to factors such as increased demand, paperwork, and media scrutiny. At the same time, the population has grown, further straining the system.
Reactions and Responses
The BMA disputes the analysis, calling it “simplistic and crude.” Dr Katie Bramall from the BMA acknowledged the variation in practice types and populations served. She emphasized that practices in university towns may have different needs compared to those in rural areas.
Helen Maguire from the Liberal Democrats criticized the government for failing to address the crisis in primary care. She called for guaranteed access to GPs within a week or 24 hours for urgent cases, warning that without improvements, there will be increased pressure on A&E departments.
NHS figures show that the summer of 2025 may be the busiest on record for general practice teams. However, data collection challenges persist, with some practices reporting inconsistencies in appointment and workforce statistics.
Perspectives from GP Surgeries
Dr Ben Davies from the Jesmond Health Partnership shared his experience with online consulting tools, which have helped improve patient access. He noted that these tools do not always feed into the systems used for data collection, leading to potential underestimates of patient interactions.
NHS Birmingham and Solihull acknowledged the need for improved data processes and are working with practices to ensure accurate reporting. Dr Steven Edgar from Millbrook Surgery emphasized the importance of providing timely access to healthcare professionals, with positive feedback from patients.
NHS South Yorkshire disputed the accuracy of the data, citing differences in how appointments are counted and recorded. These discrepancies highlight the need for standardized data collection practices across the NHS.
As the debate over GP workloads and patient access continues, the focus remains on finding sustainable solutions to ensure that all patients receive the care they need.