Understanding Brain Shape Changes and Dementia Risk
Scientists have discovered that changes in the shape of the brain as it ages could serve as early indicators of dementia. This finding opens new avenues for understanding how the brain deteriorates over time and what might signal cognitive decline.
Instead of focusing solely on individual parts of the brain, experts are now examining its overall structure and the interactions between different regions. This holistic approach is revealing key insights into how the brain ages and how these changes may be linked to cognitive impairment.
A recent large-scale study conducted by researchers from Irvine, California, and Tenerife, Spain, used brain scans to track these changes. The results showed that the brain doesn’t shrink uniformly with age. Rather, it undergoes specific shape transformations, which could be critical in identifying early signs of dementia.
Key Areas of Change
The bottom portions of the brain, responsible for essential functions like breathing and heartbeat, and the front parts, involved in certain cognitive functions, tend to expand outward. Meanwhile, the top parts, crucial for language, and the back parts, involved in visual processing and motor control, compress inward.
The distance between matching areas on the left and right sides of the brain, especially in the front, also increases. This physical pulling apart of the brain’s hemispheres can indicate reduced communication and coordination between the two sides, leading to a less efficient neural network.
These specific shape changes were found to be directly associated with poorer cognitive skills, such as reasoning. This suggests that they may serve as a clear physical sign of cognitive impairment.

As the US population continues to age, the number of dementia cases is expected to rise significantly. Current estimates suggest that the number of cases will increase from seven million to nearly 13 million by 2060. While some brain shrinkage is a normal part of aging, the average brain shrinks by about 0.2 percent per year after age 60. By the time a person reaches 80, their brain may be 10 to 15 percent smaller than it was in their 30s.
Dr. Niels Janssen, the senior author of the study and a professor at Universidad de La Laguna in Tenerife, Spain, noted that most studies focus on tissue loss in different regions. However, his team found that the overall shape of the brain shifts in systematic ways, which are closely tied to cognitive impairment.
A Massive Brain Mapping Project
To uncover how the brain’s shape changes with age, the researchers conducted an extensive brain mapping project. They started with a dataset of over 2,600 brain scans from adults aged 30 to 97, including those with dementia. They used one set of scans as their main test group and another independent set to verify their findings.
They measured the brain’s geometry in two ways. First, they placed 400 points on the outer surface of the brain to examine its global shape. Then, they measured the distances between matching points on the left and right sides, creating a detailed map of where the brain was expanding or compressing.
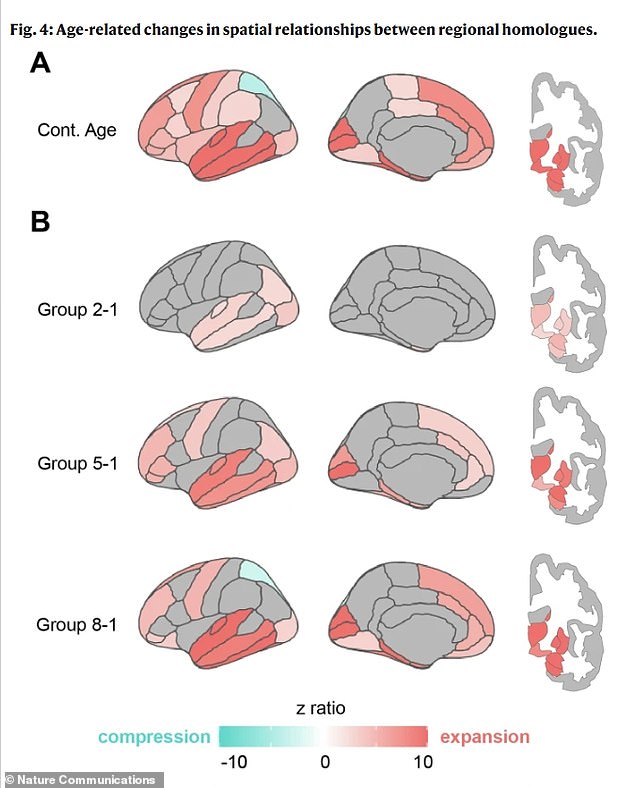
Second, they measured the distance between specific partner regions in the left and right hemispheres. Finally, they connected these physical measurements to real-world cognitive function.
Using advanced statistics, they tested whether these patterns of expansion and compression were linked to participants’ age, performance on memory and reasoning tests, and whether they had been diagnosed with a cognitive issue. This allowed them to see not just how the brain changes shape, but how those changes might affect cognitive abilities.
Specific Patterns Linked to Cognitive Health
The aging brain undergoes a dramatic reshaping, not just an overall shrinkage. Particular patterns of expansion and compression were strongly linked to brain health. For example, memory problems were associated with expansion in the temporal lobe regions, known as the memory centers.
One of the study’s most significant findings involves the entorhinal cortex, a vital hub for memory in the medial temporal lobe. The research suggests that age-related brain reshaping may physically squeeze this fragile region against the base of the skull. Since this area is where toxic tau protein first builds up in Alzheimer’s, the team proposed that mechanical and gravitational forces could be a previously unknown reason for its vulnerability.
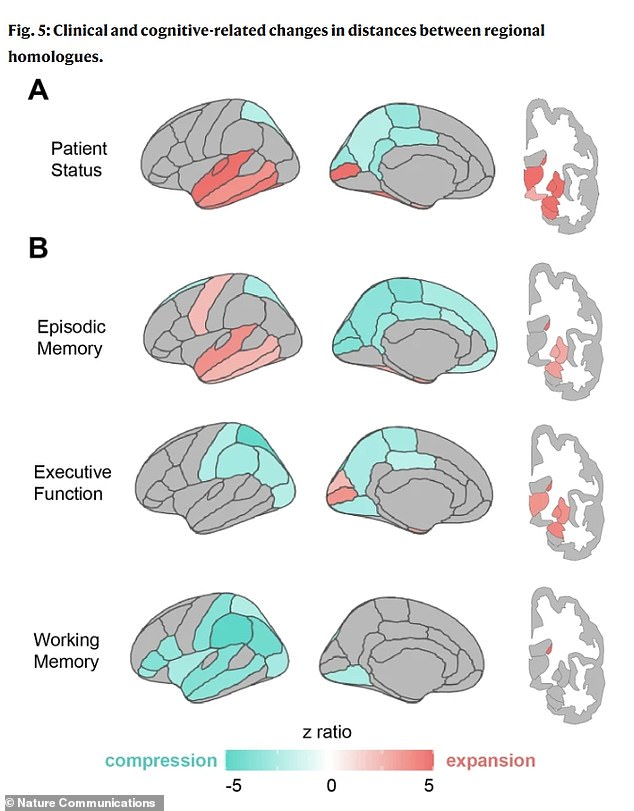
Dr. Michael Yassa, co-author of the study and a neurobiologist at the University of California, Irvine, said: “This could help explain why the entorhinal cortex is ground zero of Alzheimer’s pathology.”
Poor executive function, which includes planning and reasoning, was linked to compression in parietal regions, areas involved in integrating information and vision. The patterns seen in people with clinical impairments, such as a dementia diagnosis, were even more pronounced than in healthy aging, suggesting that this reshaping accelerates with disease.
Janssen added: “This isn’t just about measuring brain shrinkage. It’s about seeing how the brain’s architecture responds to aging and how that architecture predicts who is more likely to struggle with memory and thinking.”
Implications for Diagnosis and Treatment
The conclusion that the brain’s geometry could serve as a biomarker for dementia marks a paradigm shift in the diagnostics of Alzheimer’s disease and other forms of dementia involving shrinkage in the hippocampus and frontal cortex.
Their findings were published in the journal Nature Communications. The sagging of certain parts of the brain could be detectable long before massive cell death occurs. A routine MRI could be analyzed to detect this. A specific pattern of expansion and compression could flag a patient as high-risk years before memory tests show a clear problem.
A neurologist can examine a map of a patient’s brain and identify a pattern highly specific to Alzheimer’s, such as strong temporal lobe expansion paired with parietal compression, versus a pattern indicative of another disorder, leading to more accurate diagnoses and targeted treatment plans.





